Latest coronavirus modelling suggests Australia on track, detecting most cases – but we must keep going
- Written by Trent Yarwood, Infectious Diseases Physician, Senior Lecturer, James Cook University and, The University of Queensland
Late yesterday, epidemiologists from the Doherty Institute released what the Chief Medical Officer described as “nowcasting”: modelling that uses data from the previous 14 days to more accurately understand the present state of the COVID-19 epidemic.
In short, the findings are reassuring and suggest the inconvenience of social isolation is helping control the spread of SARS-CoV-2 in Australia.
It also indicates the spectre of “unidentified community transmission” is very unlikely indeed. This should be especially reassuring for healthcare workers, who may worry about coming into contact with COVID-positive patients presenting with a non-COVID problem.
What I don’t think it means, however, is that our outbreak control has been so effective that we should consider loosening the restrictions now.
Overseas methods, Australian data
The important thing to know is that this latest modelling uses Australian data.
One of the earlier criticisms of the Australian government’s response to COVID-19 was that the expert advice was kept behind closed doors.
When the modelling was made public, those determined to find fault (especially on Twitter) pivoted to “But it’s based on overseas data!”
That’s not a criticism that can be levelled at this latest Doherty Institute modelling, which borrows methods developed by the London School of Tropical Medicine and Hygiene but uses really recent Australian data to build some estimates.
We are likely detecting most COVID-19 cases
First, the modelling suggests there’s probably not some huge secret cohort of COVID-19 cases out there that we are not picking up due to insufficient testing.
The researchers compared the reported case-fatality rates (the proportion of COVID-19 positive people who died) in Australian states with that from a large Chinese study (1.38%).
This is then used to infer the proportion of cases with symptoms which have been found by testing.
All states/territories have case detection rates above 80% – meaning that in each state, of all the people who have COVID-19 with symptoms, we are picking up about 80% or more.
If it wasn’t for the recent outbreaks in Tasmania, then all states would be above 90%. And in fact, the overall estimated case detection rate Australia-wide is 93%. Good news!
And as time goes on, the researchers are growing more certain about this conclusion (the technical term for this is the change in the “90% confidence interval” but in plain English that means the scientists are growing more confident these estimates are pretty accurate).
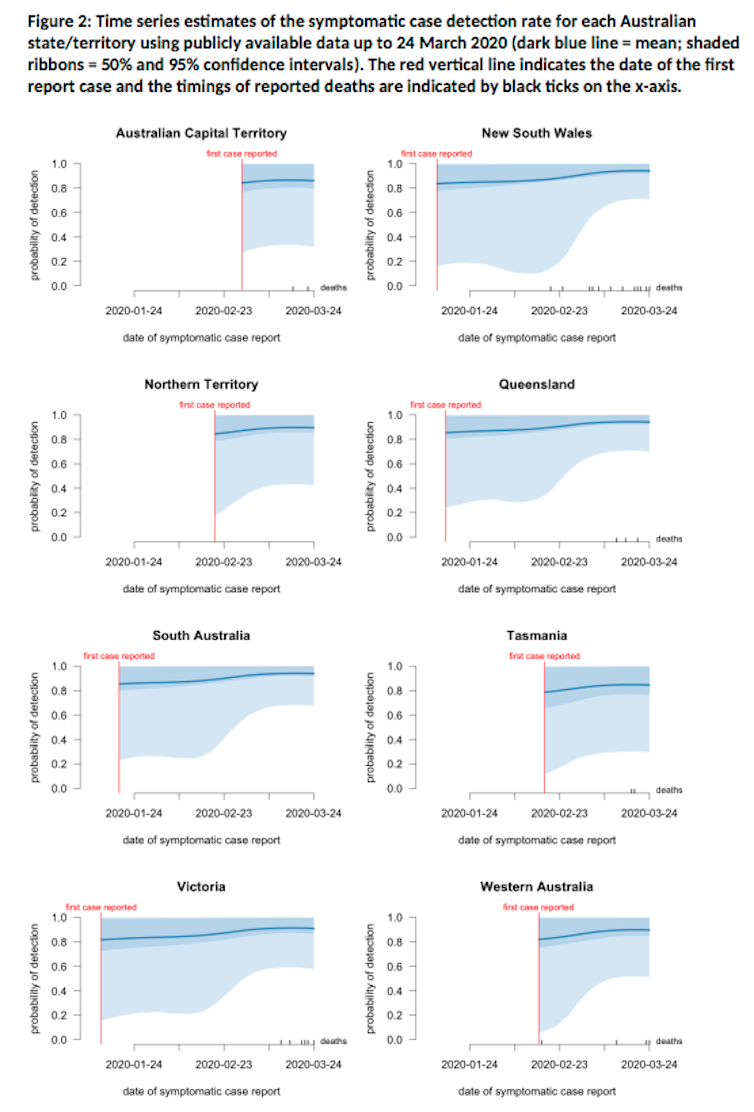 The change in the light blue shaded area means scientists are growing more confident that their estimates are accurate as more Australian data becomes available.
Doherty Institute
The change in the light blue shaded area means scientists are growing more confident that their estimates are accurate as more Australian data becomes available.
Doherty Institute
An effective R below 1: meaning social distancing is working
What scientists call the effective R is the way the virus spreads in a world where social distancing measures are in place. It refers to the average number of people each COVID-19 positive person is infecting. If it is below one, then it means the social distancing measures are working well.
The next model in the new Doherty Institute paper looks at the effective R ₀ in the six states over time.
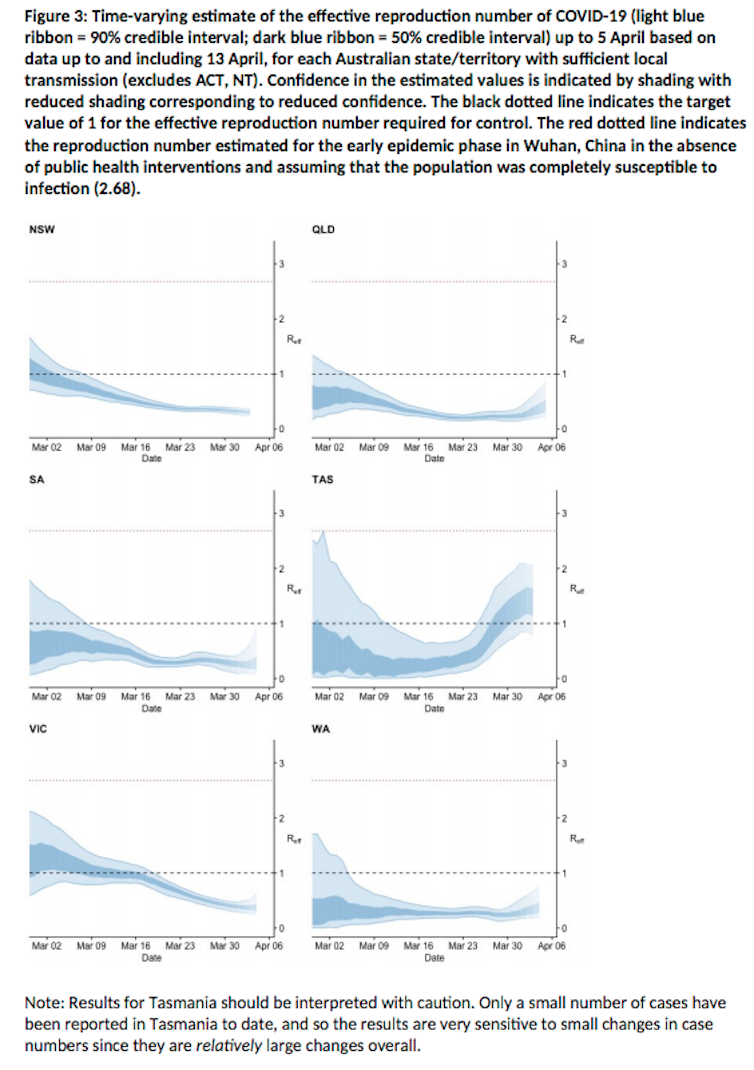 The effective R ₀ is under one in all states except Tasmania, but treat the Tasmanian data with caution: they have a small number of cases and a recent uptick, so that could be blowing out the average.
Doherty Institute
The effective R ₀ is under one in all states except Tasmania, but treat the Tasmanian data with caution: they have a small number of cases and a recent uptick, so that could be blowing out the average.
Doherty Institute
In most states, the effective R has always been below one – indicating Australia has been effective at controlling spread since the beginning of the outbreak.
However, the numbers in Tasmania should be interpreted with caution. Their overall case numbers are small and they just had a big cluster, which affected their average disproportionately.
Crucially, the study team calculated the effective R based on cases identified as local transmission, rather than imported cases. That means, in real life, the effective R may be even better than this model estimates (because this estimate doesn’t account for border restrictions and quarantine of travellers).
In other words, this modelling is aiming to look at how effective our domestic control measures are. And the answer is: they’re working pretty well.
Too soon to relax social distancing rules
The social distancing measures take time to have an effect in stopping transmission.
It would also take time to become visible if we back off too early.
See-sawing our control measures would probably be far more disruptive than holding the course for just a little bit longer, and pose a risk of coronavirus rebound.
Authors: Trent Yarwood, Infectious Diseases Physician, Senior Lecturer, James Cook University and, The University of Queensland





