Why do some people with coronavirus get symptoms while others don't?
- Written by Abela Mahimbo, Lecturer in Public Health, University of Technology Sydney
SARS-CoV-2, the coronavirus which causes COVID-19, has infected almost 2.5 million people around the world and claimed 170,000 lives.
But some people don’t even get symptoms. Recent studies suggest as many as 80% or more of those infected are “silent carriers”, showing no or very mild symptoms.
It seems children and young, healthy people are more likely to be asymptomatic.
Read more: Worried about your child getting coronavirus? Here's what you need to know
But to calculate the true proportions of people who have no symptoms right through to severe illness, testing would need to be expanded across whole populations, and this hasn’t been feasible yet.
We don’t know exactly why some people with coronavirus are asymptomatic while others develop life-threatening illness. But here’s what we know so far.
What happens when coronavirus enters your body?
Like all viruses, SARS-CoV-2 needs to get inside human cells to multiply and survive.
To do this, a particle on the outer shell of the virus latches onto a matching protein receptor, called ACE2, like a lock and key. ACE2 receptors are normally found in the lungs, kidneys, heart and the gut.
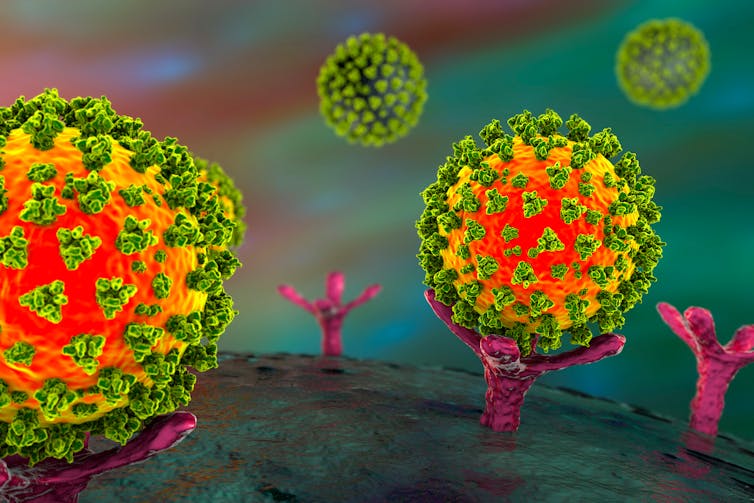 Here the SARS-CoV-2 virus (in green and orange) attaches to the ACE2 receptor (in pink).
Shutterstock
Here the SARS-CoV-2 virus (in green and orange) attaches to the ACE2 receptor (in pink).
Shutterstock
Once a person has been infected with the virus, it can take up to 14 days for symptoms to appear (if they do at all) – known as the incubation period.
The path from the point of infection can vary enormously. The body’s immune system is critical for determining this.
Having a strong immune response during the incubation period can prevent the infection taking hold, reduce the actual quantity of virus in the body and prevent it from getting to the lungs.
Some immune response basics
Our immune system offers us two lines of defence against viruses.
The first is the innate system and includes physical barriers such as skin and mucous membranes (the lining of the throat and nose), various proteins and molecules found in tissues, as well as some of the white blood cells that attack invading organisms. This immune response is general, non-specific and kicks in quickly.
Children have immature immune systems, but one hypothesis to explain why they don’t seem to get as sick with COVID-19 is that their innate immune response to coronavirus is greater than in adults.
This may lead to a reduced viral load – the quantity of virus particles that survive in the body – because they’re able to clear the virus more quickly.
 Children’s resilience to coronavirus might be due to their innate immune response.
Shutterstock
Children’s resilience to coronavirus might be due to their innate immune response.
Shutterstock
The second line of defence is the adaptive immune response. This takes longer to initiate but once established, is much more efficient at eradicating a specific infection when encountering it again.
It’s thought that very specific genetic variations in some people might play a part in how sick they get. By generating an early adaptive immune response, the body seems to recognise the virus during the incubation period and fight it off.
A person also needs to be generally healthy to be able to mount an appropriate immune response to the infection.
Read more: Why are older people more at risk of coronavirus?
After the incubation period, what determines how sick you get?
If the SARS-CoV-2 virus survives beyond the point of entry to the body (nose, eyes, throat) it might then make its way down the respiratory tract into the lungs.
In the lungs, it latches onto ACE2 receptors and continues replicating itself, triggering further immune responses to clean out infected cells. The amount of virus that gets deep into the lungs may be another important factor determining how sick you get.
As the battle between virus and immune responses proceeds, infected airway linings produce large amounts of fluid that fill the air sacs, leaving less room for transferring oxygen into the bloodstream and removing carbon dioxide.
Symptoms of pneumonia appear, such as fever, cough with sputum (phlegm) and shortness of breath.
 Fluid in the lungs makes it difficult to breathe.
Shutterstock
Fluid in the lungs makes it difficult to breathe.
Shutterstock
For some people, the immune response is excessive or prolonged and causes what’s known as a “cytokine storm”. Cytokines are a group of proteins that send signals to cells in the immune system, helping direct the response.
A cytokine storm is a catastrophic overreaction that causes so much inflammation and organ damage, it can be fatal.
In people with COVID-19, as well as the previous SARS and MERS coronaviruses, this causes acute respiratory distress syndrome (ARDS), when fluid builds up in the lungs. This is the most common cause of death from SARS-CoV-2.
Elderly people and those with chronic lung disorders are more likely to develop ARDS and therefore to die. This is currently thought to be due to these groups of people having fewer ACE2 receptors in their lungs.
Read more: What does it mean to be immunocompromised? And why does this increase your risk of coronavirus?
This seems counter-intuitive, because the virus attaches itself to these receptors. However, ACE2 receptors have an important role in regulating the immune response, particularly in managing the degree of inflammation.
So the reduced levels of ACE2 receptors in the elderly may actually make them more at risk of a cytokine storm and severe lung disease.
Conversely, children have more ACE2 receptors in their lungs which might explain why they do not get as sick.
In some cases, medications that work to suppress the immune system have successfully treated this excessive immune response in people with COVID-19.
 Older people’s immune systems respond very differently to children’s.
Shutterstock
Older people’s immune systems respond very differently to children’s.
Shutterstock
Can people without symptoms pass it on?
Some studies have indicated people with COVID-19 tend to have a high viral load just before and shortly after they start getting symptoms.
This suggests they can transmit it when they first get sick and up to 48 hours before, while they’re pre-symptomatic.
However, there is no good evidence that asymptomatic people who never develop symptoms are able to pass it on.
Researchers and clinicians are working around the clock to understand the complex relationship between humans’ immune systems and SARS-CoV-2 but it remains very much a work in progress.
Read more: What the coronavirus does to your body that makes it so deadly
Authors: Abela Mahimbo, Lecturer in Public Health, University of Technology Sydney




