Could blood thinners be a lifesaving treatment for COVID-19? Here's what the science says and what it means for you
- Written by Karlheinz Peter, Lab Head, Atherothrombosis and Vascular Biology and Deputy Director, Baker Heart and Diabetes Institute; Interventional Cardiologist, Alfred Hospital; Professor of Medicine and Immunology, Monash University, Baker Heart and Diabetes Insti
A spate of recent media headlines have described blood thinning medications – which include aspirin and warfarin – as a “breakthrough treatment” for COVID-19 that could “save lives”.
It’s early days yet but a growing body of research evidence suggests COVID-19 causes abnormalities in blood clotting, which means blood thinning drugs may have a role to play in treatment.
Here’s what the research says on this question – and how it applies to you.
Mounting evidence
When COVID-19 first emerged, it was thought the illness was a typical respiratory disease causing symptoms such as fever, sore throat, dry cough, and potentially lung infection (pneumonia) and a build-up of fluid in the lungs making it difficult to breathe.
However, as we outlined in a previous article in The Conversation, 30-70% of COVID-19 patients admitted to intensive care units, developed blood clots.
These rates of blood clotting appear to be much higher than what is expected when compared with people who are hospitalised for reasons other than COVID-19.
Blood clots in the veins often present in the legs (deep vein thrombosis) and are dislodged into the lungs (called pulmonary embolism); approximately one in four COVID-19 patients admitted to intensive care will develop a pulmonary embolism (where an artery in the lungs gets blocked).
Arterial blood clots associated with COVID-19 can lead to strokes, including in younger patients, with potentially devastating outcomes.
In addition, COVID-19 appears to cause tiny blood clots that can block small vessels in the lungs. These “micro” blood clots may be a key reason why patients with COVID-19 often have very low oxygen levels.
Blood clots appear to be associated with a higher risk of dying from COVID-19. Likewise, elevated markers of blood clotting are associated with an increased risk of admission to the intensive care unit and a worse prognosis overall.
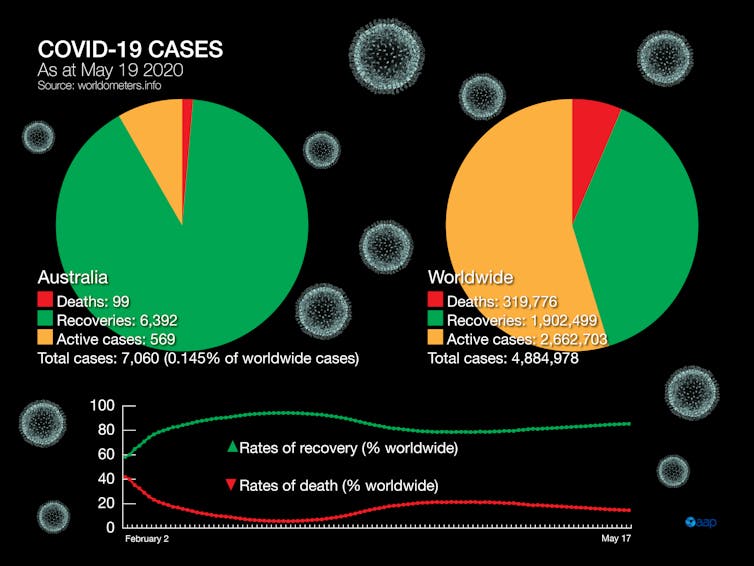 AAP Graphics/Sean Fitzpatrick
Should blood thinners be standard treatment for COVID-19 patients in hospital?
Because the rate of blood clotting is so high, all people admitted to hospital with COVID-19 should receive a low dose of blood thinner medication to prevent blood clots. This prophylactic dose of blood thinner is standard across most hospitals in Australia.
However, many blood clots in COVID-19 are occurring despite the use of low-dose blood thinners. As such, it is a question of intense discussion whether people admitted to hospital with severe COVID-19 should receive a higher-than-usual dose of blood thinners to prevent blood clots and improve clinical outcomes.
A recent study from the US suggests patients admitted to hospital and prescribed full dose blood thinners had a better chance of survival and lower chance of needing a ventilator.
However, this finding has to be confirmed before the higher dose can be generally recommended. Fortunately, several research studies are underway in Europe, the UK and elsewhere to test and answer this question definitively.
Several other blood thinner treatments are also being evaluated in people with COVID-19. Aspirin is commonly prescribed to people who are at high risk of strokes or heart attacks. There are now studies underway examining if aspirin can reduce risk of blood clotting in people with COVID-19. In the US, some stronger clot-busting medications are also being trialled in people with severe COVID-19.
It is important to note blood thinners are not without risk, as this treatment can increase the risk of bleeding. So without definite evidence to support the benefit of high dose blood thinners in all hospitalised patients with COVID-19, the decision to use higher doses of blood thinning medication outside of a clinical trial must be made on an individual basis.
AAP Graphics/Sean Fitzpatrick
Should blood thinners be standard treatment for COVID-19 patients in hospital?
Because the rate of blood clotting is so high, all people admitted to hospital with COVID-19 should receive a low dose of blood thinner medication to prevent blood clots. This prophylactic dose of blood thinner is standard across most hospitals in Australia.
However, many blood clots in COVID-19 are occurring despite the use of low-dose blood thinners. As such, it is a question of intense discussion whether people admitted to hospital with severe COVID-19 should receive a higher-than-usual dose of blood thinners to prevent blood clots and improve clinical outcomes.
A recent study from the US suggests patients admitted to hospital and prescribed full dose blood thinners had a better chance of survival and lower chance of needing a ventilator.
However, this finding has to be confirmed before the higher dose can be generally recommended. Fortunately, several research studies are underway in Europe, the UK and elsewhere to test and answer this question definitively.
Several other blood thinner treatments are also being evaluated in people with COVID-19. Aspirin is commonly prescribed to people who are at high risk of strokes or heart attacks. There are now studies underway examining if aspirin can reduce risk of blood clotting in people with COVID-19. In the US, some stronger clot-busting medications are also being trialled in people with severe COVID-19.
It is important to note blood thinners are not without risk, as this treatment can increase the risk of bleeding. So without definite evidence to support the benefit of high dose blood thinners in all hospitalised patients with COVID-19, the decision to use higher doses of blood thinning medication outside of a clinical trial must be made on an individual basis.
 The Conversation, CC BY-ND
Should I take an aspirin to prevent blood clots?
There is no evidence aspirin or other blood thinners should be taken to prevent blood clots in the general population. Also, there is no evidence blood thinners are required to prevent blood clots for people with mild COVID-19 who are isolating at home. Because blood thinners can cause bleeding, they should not be taken unless prescribed by a doctor.
It is important for people who are taking blood thinners for another reason to continue taking these medications as normal, particularly if they are diagnosed with COVID-19.
In summary, our understanding of COVID-19 and how the coronavirus attacks the body continues to rapidly evolve. Researchers from around the world are publishing data almost daily. However, not all of this research has been peer reviewed.
If you develop symptoms, the most important thing you can do is to get tested for COVID-19 and talk to your doctor about potential treatments, including hospital admission and then about blood thinning medication.
Similar to our colleagues in the UK and the US, we as doctors specialised in the field of blood clotting are indeed optimistic and hope clinical studies currently underway will show rigorous strategies for prevention and treatment of blood clotting will help to reduce severity and improve survival of patients with COVID-19.
Read more:
Coronavirus: how long does it take to get sick? How infectious is it? Will you always have a fever? COVID-19 basics explained
The Conversation, CC BY-ND
Should I take an aspirin to prevent blood clots?
There is no evidence aspirin or other blood thinners should be taken to prevent blood clots in the general population. Also, there is no evidence blood thinners are required to prevent blood clots for people with mild COVID-19 who are isolating at home. Because blood thinners can cause bleeding, they should not be taken unless prescribed by a doctor.
It is important for people who are taking blood thinners for another reason to continue taking these medications as normal, particularly if they are diagnosed with COVID-19.
In summary, our understanding of COVID-19 and how the coronavirus attacks the body continues to rapidly evolve. Researchers from around the world are publishing data almost daily. However, not all of this research has been peer reviewed.
If you develop symptoms, the most important thing you can do is to get tested for COVID-19 and talk to your doctor about potential treatments, including hospital admission and then about blood thinning medication.
Similar to our colleagues in the UK and the US, we as doctors specialised in the field of blood clotting are indeed optimistic and hope clinical studies currently underway will show rigorous strategies for prevention and treatment of blood clotting will help to reduce severity and improve survival of patients with COVID-19.
Read more:
Coronavirus: how long does it take to get sick? How infectious is it? Will you always have a fever? COVID-19 basics explained
Authors: Karlheinz Peter, Lab Head, Atherothrombosis and Vascular Biology and Deputy Director, Baker Heart and Diabetes Institute; Interventional Cardiologist, Alfred Hospital; Professor of Medicine and Immunology, Monash University, Baker Heart and Diabetes Institute




